
More evidence that low-calorie sweeteners are bad for your health
Studies show that artificial sweeteners can raise the risk of hypertension, metabolic syndrome, type 2 diabetes and heart disease, including stroke.
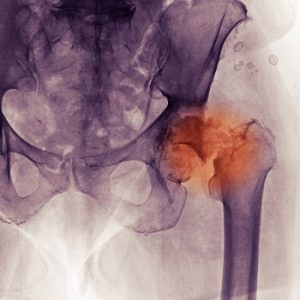
Natural Health News — Older people are often advised to lower their protein intake to lower the ‘acid load’ on their bodies.
But a new review of protein intake in older individuals reveals risks to bone health of not getting enough.
The review, which was part of new expert consensus endorsed by the European Society for Clinical and Economical Aspects of Osteoporosis, Osteoarthritis, and Musculoskeletal Diseases (ESCEO) and the International Osteoporosis Foundation (IOF) found that protein dietary protein levels even above the current RDA of 0.8g of protein per kg of body weight per day, may be beneficial in reducing bone loss and hip fracture risk, provided calcium intakes are adequate.
The review, published in Osteoporosis International, also found no evidence that acid load due to higher dietary protein intakes, whether of animal or vegetable origin, is damaging to bone health.
The key findings of the extensive literature review include:
Elderly not getting enough
» A new international expert consensus suggests that older people may need more protein – above the current RDA – to protect their bones.
» The review found that, in many older people, not getting enough was a more pressing problem than getting too much and that higher daily intakes of protein, provided there was also adequate calcium intake, did not result in as high ‘acid load’ in the body.
The review found that protein intake in those studied varied between 0.8 and 1.2 g protein/kg body weight per day and that those whose daily intake was at the higher end had healthier bones. For the elderly, higher intakes, around 1.0–1.2g protein/kg body weight per day, are acknowledged as optimum with 1.2–1.5 g/kg body weight per day recommended for some in order to preserve muscle function or in older people who are malnourished or at risk of malnutrition because of acute or chronic illness or injury.
Professor René Rizzoli, Professor at the Division of Bone Diseases of the Geneva University Hospitals and Faculty of Medicine, who led the study, stated:
“Adequate intake of dietary protein, together with calcium, is needed for optimal bone growth in children and the maintenance of healthy bone at all ages… In fact, in the elderly, we find that a common problem is not too much protein, but too little. This review of the literature confirms that a balanced diet with sufficient protein intake, regardless whether of animal or vegetable source, clearly benefits bone health when accompanied by adequate calcium intake. This is particularly important for seniors with osteoporosis, and individuals at risk of malnutrition due to acute or chronic illness, or recovering from an injury.”
The calcium factor
Throughout the review emphasises the need for adequate calcium. Earlier this year the International Osteoporosis Foundation (IOF), also launched the interactive Global Map of Dietary Calcium Intake in Adults, which shows that many populations are not getting enough calcium in their diets. The Map reflects the findings of a recent study published by an IOF Calcium Steering Committee.
Calcium is a major component of bone, accounting for between 30-35% of its mass and much of its strength. Low calcium intake has been linked to lower bone-mineral density, which increases the risk of osteoporosis and broken bones.
The amount of calcium needed varies at different stages of life. Calcium requirements are especially high in the teenage years due to the rapid growth of the skeleton, and at older age, when the body’s ability to absorb calcium declines. In older adults, bone loss occurs at a rate of about 1% per year, resulting in calcium loss of approximately 15 g per year.
The recommendations for daily calcium intake vary by country, however 800-1000 mg/day is generally recommended for healthy adults, with higher amounts recommended for teens, postmenopausal women, the elderly, and people with osteoporosis. Studies show that food rather than supplements is the generally best way to get the calcium and other bone-building nutrients we need.
Foods rich in calcium include all dairy foods (milk, yoghurt, cheeses, which are also high in protein), certain vegetables (e.g. broccoli or kale); whole canned fish with soft edible bones such as sardines; some nuts; calcium-set soy products (tofu, soy milk); and some mineral waters and tap water in hard water areas.

Please subscribe me to your newsletter mailing list. I have read the
privacy statement